Histopathology
Analysis under the Microscope
Histopathology, sometimes also referred to as cellular pathology, is a complex and crucial area of study in modern medicine.
It's an extremely detailed branch of science that focuses solely on the anatomical changes that occur in diseased tissue at a microscopic level.
This science is so specific that a histopathologist not only has to perform tests, conduct analysis and gather data, but is also responsible for interpreting the information gathered and making the final diagnosis so a patient's doctor can then move forward to manage the treatment for the specific disease.
Histo-ry
As its name suggests, histopathology is one of the subdivisions of pathology and, like its relatives, it studies various diseases to determine how they affect the different parts of the body. The primary focus of this pathology branch is bodily tissue, which translates into histo, hence histopathology.
Scientists specializing in this field look to explore the ways a tissue changes when it comes in contact with a disease and by which means a specific disease changes the tissue in an area of, or throughout, the body.
It's because of this exact science that histopathologists are able to accurately diagnose cancer, the stage it is in and the part of the body under attack, as well as other diseases, like herpes, the measles, parvo or parasitic worms.
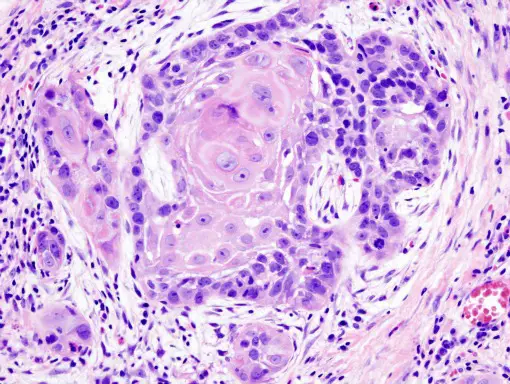
Oral cancer squamous cell carcinoma - image from Commons.Wikimedia.org
Handle with Care
Before a histopathologist can make a definite diagnosis, he or she must first go through a number of processes, starting with sample preservation and fixation.
Once a cytology sample, piece of tissue from a biopsy or surgical resection specimen comes into the lab, the scientist must handle it with the utmost care to avoid contamination or damage.
If the histopathologist does not store the specimen at the right temperature, use the right culture media, the correct stain or proper techniques, the sample may no longer be usable or the results could be inaccurate.
Of course, errors can also occur, and they usually do, if a scientist who does not specialize in histopathology attempts to analyze the sample or if the equipment utilized is not functioning properly.
One of the most common ways in which contamination of a sample occurs is when a scientist needs to use a flotation bath, a device full of water kept between 45 and 50 degrees Celsius.
This is of course the optimal temperature for algae, bacterial or fungal growth and, the addition of water only further enhances the possibility of making the specimen in the bath a breeding ground.
To avoid the risk of such contamination, a flotation bath should only contain fresh, distilled water, as the bath needs to be emptied and cleaned at the end of each day.
Stains, buffers and reagents also require storage at temperatures less than ideal for pathogenic growth so that their use does not contaminate any sample.
Technique
Histopathologists have an array of options when it comes to testing, as they can use a number of stains and various microscopy techniques to examine and analyze the sample.
Each stain has specific properties that help scientists identify a particular disease, as not every pathogen is visible with every stain.
For instance, while haematoxylin-eosin, or H and E for short, is the most common stain used for histopathological studies, the gram stain is better suited for identifying various strains of a specific bacterium.
To further clarify, a histopathologist may opt to use the Giemsa stain for detecting fungi or parasites but when looking for mycobacteria, they can elect to apply the Ziehl-Neelsen, or ZN, stain to make the pathogen visible.
Also see Microscopy Culture and Sensitivity Testing
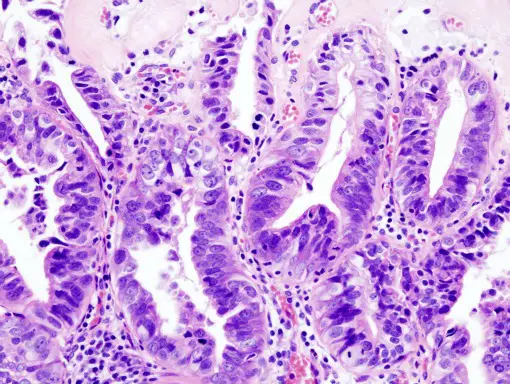
Gallbladder Adenocarcinoma - image from Commons.Wikimedia.org
Microscopy Analysis
Histopathology benefits greatly from analysis conducted under the microscope, provided the sample is pure and viable. A culture, though providing a solid foundation, does not help scientists when trying to determine whether or not a bacterial invasion occurred or if colonization took place.
In this particular instance, analysis under a microscope is necessary for a histopathologist to make an accurate prognosis.
Additionally, the microscope proves to be one of, if not the most, used and relied upon tool by scientists studying pathogens that cause tissue changes or damage, as it allows them to see the level of tissue degradation present and therefore, verify the progression of the particular disease.
Microscopy analysis is important in histopathology because it allows scientists to view tissue changes or signs of infection, even if the pathogen is not present.
A histopathologist can use a microscope to determine which pathogen is responsible for tissue damage in the event multiple infectious agents are present, thus enabling them to make a correct diagnosis.
Microscopy offers even more benefits in the field of histopathology not only because it allows for a quicker turn around time when making a diagnosis but also because it provides scientists with a means of viewing bacteria that do not cultivate, such as, Treponema pallidum, the bacterium that causes Whipple disease.
Recently, the use and importance of the microscope has increased, as histopathology processes are now including immunohistochemistry techniques, which basically allows the pathogen to show up as a fluorescent object, making detection much simpler for the scientist.
This technique is helping histopathologists to see microorganisms that were once undetectable, either because they do not cultivate, cannot be seen through traditional staining methods, do not stain well, have an unusual morphology, or simply have a small presence.
It is also allowing scientists to view missing DNA sequences on chromosomes, spot intracellular bacteria and learn more about nucleic acid and RNA.
Histopathology is a sensitive, highly detailed, pertinent field of science and medicine that provides life-changing contributions to patients and the health industry.
It is crucial that researchers, lab technicians, biologist, microbiologists and other scientists partaking in the study or diagnosis of pathogens do not overlook the importance, relevance and delicacy of this scientific branch, thus ensuring the techniques and processes are accurately performed.
The simplest of errors that go unnoticed could cause a sick patient to die or leave a significant detail about pathogens and their effects on tissue undiscovered, as well as any possible cure or treatment.
See Cytopathology and Digital Pathology also.
Our article on Cell Division is also an interesting read.
Return from Histopathology to Microscopy Applications
Return from Histopathology to MicroscopeMaster Home
Find out how to advertise on MicroscopeMaster!