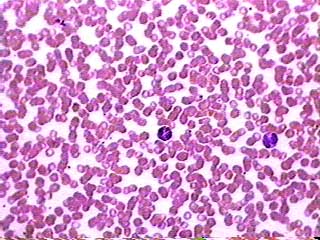
Blood Smear in Microscopy
Process and Technique
Artifacts / Refractiles
Blood Smear at 400x | In general, performing and viewing a blood smear for microscopy analysis is usually warranted when the hematology analyzers employed in laboratories indicate some abnormalities. |
Here at MicroscopeMaster, the goal is to not perform diagnoses but to briefly outline the technique and processes needed to view a blood smear under brightfield microscopy for the hobbyist who enjoys furthering their knowledge or for the student needing some clarification.
Hematology analyzers provide complete blood cell counts and differential counts of white blood cells estimating cell number but offer limited morphological information and do not identify abnormalities.
Blood Smear Process and Technique
Importantly, viewing blood smears under the microscope needs to be done shortly after blood collection employing sterile technique (**wearing gloves) from a disinfected site (wiping off 1st drop of blood). Using a high quality clean glass slide (flat, no distortions and corrosion resistant) of 75mm X 25mm and 1mm thickness is ideal. Then place the blood drop 1cm from the end of the slide.
Proceeding with the 45 degree wedge or push slide technique used in manual and automated environments, creates a monolayer blood smear. This is done in a smooth and quick motion. Fixation, staining, washing and air drying are quickly commenced.
Below is a very quick video on blood smear technique:
When staining either Romanowsky, Wright's or Giemsa stain are used or a combination thereof, usually simply Wright's stain.
Using light microscopy, imaging is done with a 10x ocular and 10x objective at first.
Increasing in progression, it is best to view smears up to a total magnification of 1000x using the 10x ocular.
Red blood cells will stain pink, platelets appear as small blue/purple and cytoplasmic granules stain pink to violet. White blood cells comprise Granulocytes which include Neutrophils, Eosinophils and Basophils and Agranulocytes which include Lymphocytes and Monocytes. Neutrophils are displayed as a deep blue/purple nucleus under the microscope.
Artifacts / Refractiles
If when viewing your dried blood smear through a microscope you are seeing refractiles, there are some questions to ask yourself and factors to consider. Firstly, what stain and technique are you using? Perhaps there is a problem with the optics and magnifications. What are these specifications? Lastly, perhaps your problem is with the specimen or your specimen preparation like poor spreading technique.
You may be seeing a drying related artifact or a stain related artifact which are usually more evident during humid summer months. Internal reflections or contamination in the sample and/or in the optics can cause refractiles. Mismatched components/mechanisms on your microscope may also be a contributing factor.
If doing a Complete Blood Count with differential, artifacts may be ignored as they should not affect your counts including red cell morphologies. An experienced observer should be comfortable in doing this so as to deliver results in a lab accurately and quickly.
Causes of refractiles: Humidity; under-fixation/late fixation; presence of water in alcohol used; excess buffer to stain, thick smear
Elimination of refractiles: Avoidance of any humidity; thin smear; dehydraton set-up
After being correctly smeared and dried, water is lost from thin areas first so as from the plasma, then water is lost from within the cells. Thicker areas dry from outside to inside. With an inactivated cell membrane, loose water can no longer disperse from the cell unless in the case of rupture which will then easily destroy cell morphologies. A cause of refractiles due to inadequate drying can be trapped water in an inactive cell membrane.
Refractiles may be avoided with more rapid heating and then drying before staining. Perhaps simply waving the slide around immediately after placing the smear to speed drying will prove sufficient.
An artifact caused by staining is more difficult to remedy.
Live Blood Analysis Refractiles
In live blood analysis, much the same questions and factors can be considered. A new piece of optical equipment/dye may alter your signal-image. For example, the autofluorescense in hemoglobin may disrupt your emission signal from your fluorescent dye.
If halos are present causing refractiles because of autofluorescence then you should consider the addition of either trypan blue, methylene blue or Toluidine blue to your stain.
A blood smear is easily sampled and features of blood are very observable which is especially valuable when disease is present. It is vital to keep in mind sterility, quality control and proper technique in handling your blood smear.
Optical microscopy offers the ability to gather information and aid in continued research. Thus, MicroscopeMaster hopes to have shed some light.
Of Interest:
1/ Live Blood Analysis is met with some skepticism
2/ Cell Staining in Microscopy
4/ Hematuria
6/ Microscopy Culture and Sensitivity
Here is a great microscope to view live blood:
OMAX 40X-2000X USB3 14MP PLAN Trinocular Darkfield Super Bright LED Lab Microscope
Return to learning but Red Blood Cells
Return from Blood Smear to Microscope Slide Preparation
Return to Microscopy Research Home
Find out how to advertise on MicroscopeMaster!