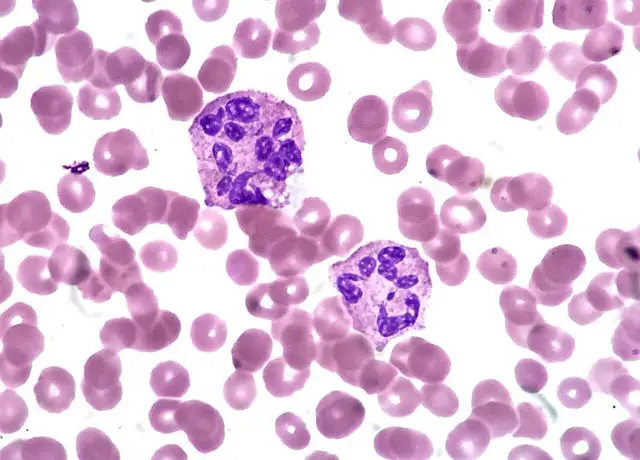
Neutrophils and Microscopy
Procedure, Observations and Discussion
In human beings, neutrophils (neutrophilic polymorphonuclear leukocytes) are the most abundant white cells given that they make up about 60 percent of the total leukocytes (white blood cells).
Through a process known as cell signaling, they have been shown to be the first leukocytes to arrive at the inflammatory sites to defend the body against such microorganisms as bacteria and fungus.
At the site of infection, neutrophils typically ingest the pathogen through a process known as phagocytosis and captured within the phagocytic vacuole. This is then followed by the release of digestive enzymes in to the vacuole to destroy and thus neutralize the pathogen or other foreign particles.
Microscopy
While there are more advanced techniques such as Immunofluorescence microscopy that can be used to view neutrophils, these cells can also be viewed using a simpler blood smear technique.
https://www.flickr.com/photos/euthman/36831145373
Requirements
- A compound microscope
- A microscope glass slide (2 or 3)
- Giemsa stain
- Blood lancet/pricking needle
- Drying rack
- 70% alcohol
- 7- 7.2 pH buffer
Procedure
- Using 70 percent alcohol, clean the finger tip (the middle or ring finger) and prick using the prick needle
- Using a cotton swab with alcohol, wipe away the first drop of blood
- Place a drop or two of blood on to the center of a clean microscope glass slide (prepare two separate slides for a thick and thin film)
- Using another clean slide held at a 45 degree angle, spread the blood on one of the slides to create a thin film
- For the second preparation, use a clean wire loop or laboratory stick to spread the blood drops to a diameter of about 1.5 cm.
- Allow the slides to dry completely (air dry)
- Fix the thin slide using 100 percent methanol
* Make sure the slides are completely dry before staining.
Staining
- Place the slides in a jar of Giemsa stain for about 50 minutes
- Rinse the slides several times in plain buffer and place them on a standing rack to dry
- View under the microscope without a cover slips (add immersion oil to view under 1000x)
See Also: Cell Staining
Observation
When viewed under the compound microscope, students will easily detect red blood cells given that they will be the most abundant cells. However, students will also be able to see neutrophils, which will not only look bigger than the other cells, but also have several lobes (2 to 5 lobes).
When viewed under high magnification, students will notice that there are very few of this type when compared to the red cells per given field of view.
Discussion - Neutrophils
Whenever pathogens intrude and enter the tissue of the host, the epithelium, mast cells and resident tissue macrophages are activated and start releasing chemokines (C5a, interleukin-8) that in turn attract and activate neutrophils.
Through a series of events, neutrophils travel up the chemokine gradient towards the infected area by adhering and emigrating through the vascular endothelium in a process refered to as chemotaxis.
Although they typically destroy pathogens through phagocytosis, they can also achieve this by using neutrophil extracellular traps (NETs) outside the cell. NETs are formed out of processed chromatin that is combined with granular and specific proteins in the cytoplasm.
When released out of the cell, NETs traps the pathogen, which allows neutrophils to control the spread of the pathogen.
Related: Basophils, Lymphocytes, Monocytes, Eosinophils, Mast Cells, Macrophages
Return from Neutrophils to White Blood Cells Main Page
Return to Cell Biology Main Page
Return to MicroscopeMaster Home
Find out how to advertise on MicroscopeMaster!