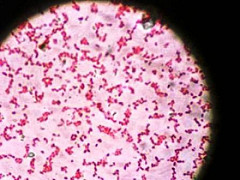
Campylobacter
Classification, Jejuni, Infection and Gram Stain
Overview
The genus Campylobacter is composed of Gram-negative bacteria species that are naturally occurring in the environment.
These bacteria are the most common cause of food poisoning and have been shown to colonize oral cavities, the mucosal surfaces of the intestinal track as well as the urogenital tract of a variety of animal and birds. As such, Campylobacter bacteria are responsible for several diseases including food-borne diarrhea.
The following are some of the species that belong to this genus:
- C. coli
- C. gracilis
- C. jejuni
- C. lari
- C. rectus
- C. curvus
Classification
Domain: Bacteria - Like many other types of bacteria, the genus Campylobacter belongs to the domain Bacteria that consists of prokaryotic microorganisms.
Phylum: Campylobacter belongs to the phylum Proteobacteria. This is a major phylum composed of Gram-negative bacteria and includes such bacteria as Helicobacter. Some books refer to this as the epsilon-subdivision
Class: Epsilonproteobacteria - this is a class of proteobacteria and consists of a few genera such as Helicobacter and Campylobacter. Most of the bacteria that belong to this class are either spirilloids or curved in shape.
Family: Campylobacteraceae - Class Campylobacteraceae is one of the most diverse families of class Epsilonproteobacteria. Apart from Campylobacter, this class is also made up of Arcobacter and Sulfurospirillum.
* Campylobacter is closely related to genera Helicobacter and Wolinella.
Campylobacter Microbiology
Following the extensive revision of Campylobacter taxonomy, the genus has been shown to include over 22 species. C. Jejuni and C. coli are some of the most common species belonging to the genus since they are primarily responsible for gastroenteritis in human beings.
Recently, however, there are several emerging species that have been associated with such infections.
These include:
- C. hyointestinalis
- C. concisus
- C. sputorum
Ecology/Habitat
Campylobacter bacteria have been shown to thrive in habitats with lower levels of oxygen (below 5 percent). As such, they are found in the mucosal surfaces of a variety of animals and birds which provide this condition.
In addition to the favorable level of oxygen, this environment also provides a conducive temperature range that favors growth and multiplication. Compared to other species, C. jejuni is suggested to have evolved thus enabling the bacteria to colonize and survive in the intestinal mucosa of birds and mammals.
In the intestinal mucosa of birds, the C. jejuni has been shown live as a commensal. It benefits from the conditions of the habitat without causing harm to the host.
In the intestinal mucosa of mammals, where the temperature is relatively lower when compared to that of birds, these organisms act as pathogens ending up causing harm.
* While Campylobacter is normally found in the mucosal surface of birds and animals, they can also be isolated from other environments including contaminated water and such animal products as milk and meat. However, they do not thrive in such environments.
* Although some species may be often found in given hosts, Campylobacter species are not exclusive (host specific).
Physiology: Members of Campylobacter have the following biochemical traits:
- Low G+C content (guanine-cytosine content) - GC ration is about 30 percent
- Ideal/optimal growth temperature range between 30 and 42 Degrees Celsius
- Do not form spores
- Are oxidase positive
- Are microaerophiles - Because they do not ferment substances for their energy, Campylobacter requires oxygen for respiration. However, Campylobacter requires low levels of oxygen in their environment to grow and reproduce
- Obtain energy through respiration
* Campylobacter species are very sensitive to a variety of external conditions (UV light, heat, salt etc). They are unable to multiply and thrive outside the host's body meaning that they cannot reproduce on such samples as meat etc.
Some of the other characteristics of Campylobacter include:
- Dimensions of between 0.5 and 5 um in length and 0.2 and 0.9 Um in width
- Spiral movement
- Polar flagella
- DNA ranges between 1.6-1.7 Mbps and contains a high content of adenine and thymine
- Cannot grow where water activity concentration is below 0.987
Campylobacter Jejuni
C. jejuni is one of the most popular members of genus Campylobacter. This is largely due to the fact that the bacterium is the leading cause of bacterial diarrhea as well as the causative agent of gastroenteritis among human beings and animals.
Biology
C. jejuni is a member of the 16S rRNA superfamily VI of spiral, microaerobic bacteria. This gene sequence is used for identification purposes and includes some other members belonging to Helicobacter and Arcobacter.
Physiology/Metabolism
C. jejuni has evolved to colonize the gut of various organisms (hosts) such as birds and mammals. As they are not the only microbiota in these environments, they use mechanisms that are different from those of other microbiota to obtain nutrients and thrive.
As the C. jejuni does not possess most of the metabolic pathways required to use such sugars as glucose and galactose as well as various other carbohydrates needed to support growth and multiplication, it still remains unclear to scientists how the bacteria compete with other microbiota in this environment. Regardless, it has been shown to efficiently use various metabolic pathways for survival.
A good example of this is the citric acid cycle intermediates as well as various other amino acids. Here, the bacterium readily makes use of such amino acids as aspartate, serine, and glutamate among others to obtain energy for survival.
Also, the bacterium is capable of metabolizing the I-fucose sugar in addition to using unique mechanisms to obtain certain transition metals that are necessary for life (iron etc). The mechanisms make it possible for C. jejuni to grow and multiply in the gut of various hosts where other microbiotas live.
* Despite lacking various enzymes required for metabolism, C. jejuni uses the glycolytic pathways to obtain energy.
Some of the amino acids used as a source of nutrients by the bacteria include:
- Serine
- Aspartate/glutamate
- Proline
- Asparagine
- Glutamine
C. jejuni also uses the following short chain fatty acids:
- Acetate
- Lactate
Infections
Like C. coli, C. jejuni is a food-borne pathogen which means that it is transmitted to an individual through contaminated food. However, they can also be transmitted through contaminated water or fruits etc.
Once the bacterium is ingested, it uses chemotaxis to detect chemical gradient and their flagella to move towards their desired environment. According to studies, some of the most common chemoattractants include mucin, L-fucose, and L-serine among others.
Chemotaxis and the presence of flagella have therefore been shown to be important virulence factors. Apart from the ability to determine where to move through chemotaxis, C. jejuni, as well as C. coli, are capable of attaching to the surface cells in their environment thus allowing the bacteria to successfully colonize these environments.
This is achieved through the production of fimbriae which is the mechanism through which the bacteria adhere to surface cells.
Gastroenteritis
Following the initial infection, incubation takes between 24 and 72 hours. This infection causes the patient to develop acute diarrhea which is followed by such signs/symptoms as chills, myalgia, fever, and headache depending on the patient and level of infection.
During this period (when symptoms present themselves) patients usually have several bowel movements (8 to 10 bowel movements) throughout the day. Here, diarrhea can either be loose or watery depending on the patient/level of infection. In some patients, however, diarrhea may contain visible blood (this is not obvious in most cases).
* Usually the infection clears within a week even without treatment. However, it may persist among some patients particularly those with compromised immunity (such as HIV infection).
Apart from gastroenteritis, there are a few other infections/complications associated with C. jejuni.
These include:
Invasive Disease
While bacteremia is not common with C. jejuni, it has been observed in certain patients; particularly the elderly as well as patients infected with HIV.
Here, the bacteria move into the bloodstream where it causes further infection by releasing toxins. For patients with invasive disease, bacteremia enhances mortality rate due to the complications that arise.
In rare cases, C. jejuni sepsis has been shown to result from transmission from other animals. A good example of this is a case where C. jejuni infection was transmitted from a puppy to a 3-week old infant. This discovery proved that it is possible for animal infections with C. jejuni to be passed onto human beings.
Guillain-Barre Syndrome (GBS)
GBS is a form of neuromuscular paralysis that affects 1 to 2 in 100,000 people annually across the globe. Essentially, it is an autoimmune disease where the immune system of the body attack and cause inflammation to the nerves ultimately resulting in muscle weakness.
Following a series of studies, researchers discovered that C. jejuni can, and does, trigger GBS. Here, researchers discovered that in cases where C. jejuni acts as the pathogenic factor in this condition, lipopolysaccharide present on its surface act as the antigenic factors that induce/trigger the disease.
For those suffering from this condition, some of the early symptoms include motor and sensory deficits at the lower extremities that gradually spread to other parts of the body. For some patients, the symptoms can persist with increased and severe impairment of the neurological system.
In animals, C. jejuni is responsible for the following infections/diseases:
- Diarrhea in dogs and cats
- Haemorrhagic vaginal discharge in dogs (such as German Shepherd)
- Miscarriage and enteritis in sheep and cattle
- Colitis among weaned pigs
- Anorexia and diarrhea in swine
- Hepatitis and yellow diarrhea among some bird species (such as psittaciforms and passeriforms)
* While studies are ongoing, C jejuni, as well as several other members of Campylobacter have displayed the ability to produce enterotoxin and cytotoxin. These toxins contribute to the various infections observed in both human beings and animals.
* Endotoxins - Like many other gram-negative bacteria, Campylobacter species such as C. jejuni produce Lipopolysaccharides as a constituent of their outer membrane.
This endotoxin plays an important role as the primary surface antigen that enhances the physical integrity and functioning of the bacteria's outer membrane. In addition, the glycolipids also contribute to the pathogenic activities of the bacteria.
Prevention
Given that Campylobacter pathogens are transmitted through contaminated food and water, infection can be easily and significantly prevented by improving hygiene.
This should involve the following routines:
- Properly wash fruits before eating them
- Washing hands with soap and water before and after eating
- Washing hands with water and soap after using the toilet, petting animals, caring for the sick and touching garbage etc
- A minimum of 165°F when cooking meats and other animal products (sausages etc.)
- Avoiding untreated water - It is always recommended to boil water if water comes from untreated sources etc.
Treatment
Treatment of Campylobacter-related diarrhea starts with the replacement of lost body fluids and electrolytes. This is particularly important given that a lot of fluids and electrolytes are lost through diarrhea (especially watery diarrhea). To prevent dehydration, physicians will often prescribe oral/intravenous fluids
Treatment may also involve the use of such antibiotics as levaquin and azithromycin.
Gram Stain and Microscopy
Gram Stain Protocol
Specimens/Requirements
- Bacterial sample (Campylobacter)
- Gram stain solutions (Crystal violet, Grams iodine, acetone-alcohol, safranin)
- Glass slide
- Pipette/applicator stick
- Inoculating loop
- Bunsen burner
Procedure
- Using the pipette, place a drop of the sample at the middle of the glass slide
- Air-dry the slide and pass over the Bunsen burner flame several times to fix the smear
- Flood the smear with crystal violet solution and allow to stand for about 30 seconds
- Decant the primary stain and then rinse the slide with water (gently)
- Rinse any excess water on the slide and flood the smear with fresh iodine
- Rinse with water and add a few drops of the alcohol (decolorizer)
- Remove excess decolorizer by slanting the slide and gently rinse with water
- Flood the slide with the counterstain (safranin) and allow to stand for about 30 seconds
- Rinse excess safranin with water and allow the slide to dry
- Examine the slide under the microscope
See more on Gram positive and Gram negative bacteria
Observation
Campylobacter is a Gram-negative bacteria. As such, they will appear as a pink/purple comma or as s-shaped cells when viewed under the microscope.
Return to Prokaryotes main page
Return to Unicellular Organisms - Discussing Bacteria, Protozoa, Fungi, Algae and more
Return to Proteobacteria - Functions, Diseases, Characteristics and Structure
Return to Bacteria under the Microscope main page
Return from Campylobacter to MicroscopeMaster home
References
Julian M. Ketley (1997). Pathogenesis of enteric infection by Campylobacter.
Martin Stahl, James Butcher and Alain Stintzi (2012). Nutrient acquisition and metabolism by Campylobacter jejuni.
Filomena Iannino, Guido Di Donato, Enzo Ruggieri, Stefania Salucci,
Fabrizio De Massis and Elisabetta Di Giannatale (2017). Campylobacter infections, a significant issue of veterinary urban hygiene: dog‑related risk factors.
Alessio Facciolà, Emanuela Avventuroso, Giuseppa Visalli and Pasqualina Laganà (2017). Campylobacter: From Microbiology to Prevention. Journal of preventive medicine and hygiene · June 2017.
Links
https://www.britishpoultry.org.uk/introduction-to-campylobacter/
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5584092/
https://www.ncbi.nlm.nih.gov/pubmed/1625311
Find out how to advertise on MicroscopeMaster!
![Campylobacter: CDC [Public domain], via Wikimedia Commons, Source: https://phil.cdc.gov/Details.aspx?pid=16870 Campylobacter: CDC [Public domain], via Wikimedia Commons, Source: https://phil.cdc.gov/Details.aspx?pid=16870](https://www.microscopemaster.com/images/Campylobacteriosis.png)