Macrophages
Definition, Function, vs Monocytes, vs Neutrophils etc.
Definition: What are Macrophages?
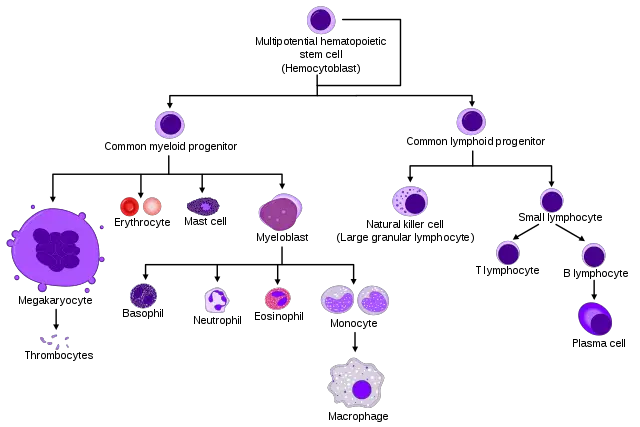
Essentially, macrophages may be described as large white blood cells found in body tissues. In blood, they were traditionally said to exist as monocytes that differentiate into different types once they leave blood circulation and migrate to damaged tissue.
The type is largely dependent on the anatomical location in which they are found in the body. In the liver, they are known as Kupffer cells but referred to as adipose tissue macrophages in adipose tissue.
Although they are well known for their effective phagocytic nature, studies have shown their functions to go well beyond immunology. Tissue repair and metabolism are examples of some of their non-immunological functions in different tissues of the body.
As cells that function in virtually all body tissues, macrophages are highly flexible, which allows them to efficiently perform their functions and respond appropriately.
Some of the other types of macrophages include:
- Langerhans cells
- Microglia
- Sinus histiocytes
- Intraglomerular Mesangial cells
- Alveolar macrophages
* The term "macrophage" comes from the Greek word "Makro" which means big and "Phagein" that means eat.
Origin
For a long time, macrophages were described as monocytes found in tissue. As such, they were largely viewed as the differentiated forms of monocytes residing and functioning in different tissues of the body. New studies, however, are showing that this is not necessarily the case.
According to recent studies that focused on Ly6chimonocytes, it was discovered that these monocytes could migrate into tissue and remain undifferentiated. In the extravascular tissue, the monocytes were shown to be capable of picking up antigen and transporting them to the lymph nodes without differentiating into macrophages.
Rather than originating from monocytes found in circulation, many studies are now finding more evidence that a large proportion of macrophages found in tissue originate from embryonic precursors of the yolk sac or fetal liver.
Here, macrophages were first shown to originate from the yolk sac and spread in the embryo. Following fertilization, they were shown to originate from hematopoiesis in the liver of the fetus.
* In adults, renewal of macrophages is suggested to originate from the bone marrow which shows that a given population of macrophages may still arise from the differentiation of monocytes.
* In mice, macrophages originate from the yolk sac (in the embryo) and fetal liver during embryonic development. They spread to different body organs and continue to renew themselves within the tissue in which they reside.
Monocytes Vs. Macrophages
Given that a population of macrophages is suspected to originate from monocytes in adults, the two types of white blood cells are closely related and share a number of similar characteristics.
Produced in the bone marrow, monocytes are found in circulating blood where they have a brief life span of about 24 hours in healthy individuals. In the event of an infection, however, some monocytes have been shown to be capable of migrating into various tissues where they carry out their function without any physiological or physical changes.
In other cases, however, monocytes migrate from blood to tissue where they differentiate to form macrophages that can reside in different body tissues for longer.
As cells of the innate immune system, monocytes also act as the front line of defense in the body and are therefore activated to respond whenever invading microorganisms are present in the body. Given that they can be found in circulating blood, they are able to respond to any foreign/invading microorganisms rapidly.
* Monocytes can also differentiate into dendritic cells that process and present antigen material to T cells.
* Monocytes secrete cytokines and chemokines that activate other types of white blood cells to respond.
There are three types of monocytes which include:
- Classical monocytes that are characterized by CD14 receptors on their surface
- Non-classical monocytes characterized by both CD16 and CD14 surface receptors
- Intermediate monocytes characterized by CD14 surface receptors as well as a few CD16 receptors
For the most part, the differences between monocytes and macrophages are based on their location and structure. Whereas monocytes are typically found circulating in blood (for 1 or 2 days), macrophages are found in various body tissues/extracellular fluid.
On the other hand, monocytes are small in comparison to macrophages which are the largest of all white blood cells. With regards to size, here, monocytes range between 7 and 9um in diameter while macrophages are about 21um diameter in size.
Differences between the two are also characterized by surface molecules. For instance, whereas monocytes only contain CD14 and CD16 surface receptor molecules, macrophages contain several more surface molecules including MAC-1, MAC-3, CD68, Cd11b, and Lysozyme M among a few others.
* Like monocytes, macrophages also contain granules that contain various enzymes.
Lymphocytes Vs. Macrophages
One of the main differences between macrophages and lymphocytes is that whereas lymphocytes destroy invading microorganisms in a specific manner, macrophages, which are phagocytes, destroy microorganisms through phagocytosis in innate immunity.
As members of the adaptive immunity, lymphocytes use specific responses to protect the body. For instance, by activating B cells, T cells stimulate B cells to produce antigen-specific antibodies that destroy microorganisms.
Neutrophils Vs. Macrophages
Like neutrophils, macrophages are also involved in innate immunity. In the presence of invading microorganisms, macrophages will respond as phagocytes where they destroy microbes by engulfing them.
Unlike neutrophils, however, macrophages are agranulocytes and function in various tissues (whereas neutrophils function in circulation). Differences between the two can also be seen in their structures and morphology.
Whereas neutrophils contain a multi-lobed nucleus, macrophages, which are larger in size, contain a nucleus that is spherical in shape. As well, neutrophils make up a significant proportion of white blood cells (50 to 70 percent) while macrophages make up less than 10 percent of the total white cell count.
* Macrophages and neutrophils can also be differentiated based on their respective surface receptors. Whereas neutrophils contain Ly6G+ and MPO+ on their surface, macrophages contain EMR1+, CD107b+, and CD68+ on their surface.
Functions
As already mentioned, macrophages play several functions in the body. While they are part of the immune system and play a role in defending the body from various invading microorganisms, macrophages are also involved in a number of other non-immunological functions that range from homeostasis functions to tissue regeneration.
Immunity Functions of the Macrophage
With regards to immunological functions, macrophages are involved in both innate and adaptive immunity. Essentially, however, macrophages are part of the innate immune system and part of the front line of defense. As such, they are among the first immune cells to respond to infections/inflammation in the body.
While various macrophages in specific body tissue respond, monocytes in blood also undergo changes to produce macrophages in order to increase the supply to the affected site.
At the affected site, macrophages destroy invading microbes through phagocytosis. Here, target cells are engulfed and destroyed by various enzymes within the macrophages (in the phagosome).
Apart from engulfing and destroying bacteria and various other microbes in the body (by disintegrating them within the phagosome) some of the macrophages also act as scavengers and play an important role in the removal of dead cells and necrotic ones. This is an important function of macrophages in that it helps in waste removal that would otherwise affect the normal functioning of other healthy cells.
* In the body, the type of macrophage formed from a monocyte is largely dependent on the type of cytokines that stimulate the differentiation. For instance, whereas the presence of interferon-y results in the production of macrophages that destroy invading microbes through phagocytosis, glucocorticoids cause monocytes to differentiate into regulatory macrophages.
Regulation of the Immune System
Macrophages have been shown to help regulate the immune system through the release of IL-10 (interleukin 10). Through the release of this cytokine in high amounts, immune responses are suppressed which plays an important role in limiting inflammation.
By studying this action, researchers are confident that there is a way to produce treatment for various autoimmune diseases.
Adaptive Immunity
Apart from innate immunity, where macrophages destroy microorganisms through phagocytosis, macrophages are also involved in adaptive immunity. Here, macrophages alert other cells of the immune system (e.g. lymphocytes) of the invasion (microbial invasion in the body).
Following the ingestion of invading microbes through phagocytosis, macrophages present antigens, which in turn activate the appropriate lymphocytes (T helper cells). In turn, these cells activate the production of cytotoxic T cells that attack and destroy the infected cells along with the invading microbes.
Here, B cells are also activated to produce the appropriate/corresponding antibodies that not only target and destroy the organism possessing the antigen, but also keep a memory of the antigen which allows it to target any cells that possess the antigen over time. In the event of recurring infections, the antibodies are able to respond effectively having identified the antigen.
Bone Remodeling
Bone remodeling is an important process that ensures that bones are properly formed in the body. Mesenchymal cells known as osteoblasts are involved in the formation of bones in the body. However, excess deposits may result in increased mineralization (osteopetrosis).
Here, cells known as osteoclasts or osteoclast macrophages are involved in bone degradation through the release of acidic enzymes (acidic collagenolytic enzymes). The activities of osteoblasts and osteoclasts play a role in bone remodeling allowing for proper bone development.
Signal exchanges between the two types of cells have also been shown to play an important role in bone development. In the event of apoptosis of osteoblasts due to bone damage, osteoclasts are recruited to the bone surface along with molecules that promote the differentiation of these cells to form osteoblasts (which other molecules (IL-33) inhibit the formation of more osteoclasts).
This promotes bone formation allowing for the damaged part of the bone to be repaired. On the other hand, through the production of such molecules as the semaphorin 4D, osteoclasts inhibit bone formation thus preventing any further deposits that may affect proper development.
Here, then, macrophages play a crucial role in bone development by influencing the activities of osteoblasts.
Erythropoiesis
Erythropoiesis refers to the process through which red blood cells are formed in the bone marrow. It is worth noting that red blood cells are broken down by macrophages that reside in the spleen and the liver. However, splenic red pulp macrophages promote the transport of iron to the bone marrow. Then, parts of degraded red cells are recycled for the formation of new red blood cells.
In the erythroblastic island (this location was discovered recently) macrophages produce ferritin that is released (following exocytosis) and engulfed by committed erythroblasts through a process known as endocytosis.
Within the erythroblasts, acidification and proteolysis processes result in the release of iron from ferritin which is in turn used for the production of heme.
* Apart from promoting Erythropoiesis, macrophages (particularly those of the liver and spleen) play an important role in the removal of senescent red cells from circulation (after about 120 days).
This, along with Erythropoiesis ensures that a constant number of red cells is maintained. Therefore, macrophages can be said to play a crucial role in the life cycle of red blood cells.
Synaptic Pruning
Macrophages located in the brain (microglia) and spinal cord (originated from the yolk sac) play an important role in brain development. In a process known as synaptic pruning, microglia clear any immature and defective synapses, which in turn promote proper synaptic maturation.
According to research studies, dysfunctional microglia has been associated with various disorders in the brain and spinal cord. In some cases, it has been associated with the development of Alzheimers in some patients showing that macrophages play a crucial role in brain development as well as the proper functioning of the neural system.
Wound Healing
In the event of tissue injury, the release of IL-4 stimulates the production of macrophages that are involved in the conversion of arginine to ornithine. The ornithine, through several stages produce collagen and polyamines that are involved in the formation or extracellular matrix that provides structural support for cells. This promotes wound healing of the injured part of the body.
* The exploitation of macrophages involved in wound-healing has been shown to negatively affect the wound healing process, which has, in turn, allowed researchers to get a better understanding of these cells.
Tissue Regeneration
In virtually all body tissues, macrophages are involved in tissue/organ regeneration. According to studies that were conducted using mice, researchers discovered that macrophages were capable of producing signals that enhanced angiogenesis and tissue regeneration.
In the absence of these cells, myocardia regeneration was negatively affected while fibrotic scars were shown to develop. Here, however, communication between macrophages and a number of other cells is essential.
Through communication between macrophages and cells of the blood vessels, regeneration of the peripheral nerves was shown to take place. This process has been observed in a number of organisms including salamanders where macrophages are involved in the regeneration of limbs.
Some of the other important functions of macrophages include:
- Iron recycling in the production of red blood cells
- Thermogenesis - Heat production
- Metabolism
- Lung homeostasis
Also, Cell differentiation
Return to White Blood Cells and more information here - Leukocytes
Return from Macrophages to MicroscopeMaster home
References
Daisuke Hirayama, Tomoya Iida, and Hiroshi Nakase, (2018). The Phagocytic Function of Macrophage-Enforcing Innate Immunity and Tissue Homeostasis. NCBI.
Paola Italiani and Diana Boraschi. (2015). New Insights Into Tissue Macrophages: From Their Origin to the Development of Memory. Immune Network.
Slava Epelman, Kory J. Lavine, and Gwendalyn J. Randolph. (2014). Origin and Functions of Tissue Macrophages.
Thomas R. L. Klei et al. (2017). From the Cradle to the Grave: The Role of Macrophages in erythropoiesis and erythrophagocytosis. Frontiers in Immunology.
Toshiaki Ohteki and Yasutaka Okabe. (2018). Introduction: Special Issue—The Origins of Macrophages and Their Roles Beyond Immunology.
Steven D. Douglas. Chapter 67. Morphology of Monocytes and Macrophages .
Links
https://www.cell.com/immunity/comments/S1074-7613(16)30053-X
https://www.researchgate.net/publication/315830016_Difference_Between_Monocyte_and_Macrophage
https://www.immunology.org/public-information/bitesized-immunology/cells/macrophages
Find out how to advertise on MicroscopeMaster!
![Micrograph showing pulmonary macrophages in a bronchial wash specimen by Librepath [CC BY-SA 3.0 (https://creativecommons.org/licenses/by-sa/3.0)] Micrograph showing pulmonary macrophages in a bronchial wash specimen by Librepath [CC BY-SA 3.0 (https://creativecommons.org/licenses/by-sa/3.0)]](https://www.microscopemaster.com/images/Macrophages_in_bronchial_wash_specimen_--_very_high_mag.jpg)